May is Osteoporosis Awareness Month! Statistics show that over 2 million Canadians are affected by osteoporosis. If you, or someone you know, has been diagnosed with Osteoporosis, read our post to learn more about the disease. Learn some of the tips and advice that our Oakville chiropractor gives to patients with osteoporosis!
Click Here To Learn More About Osteoporosis
What Is Osteoporosis
Osteoporosis means ‘porous bone’. When our bodies don’t make enough bone, or lose too much bone, naturally the bones become more porous and therefore weaker. Losing bone mass is not painful and occurs over a number of years, so by the time it becomes symptomatic, it is often fairly advanced. At least 1/3 of women and 1/5 of men will break a bone due to osteoporosis in their lifetime!
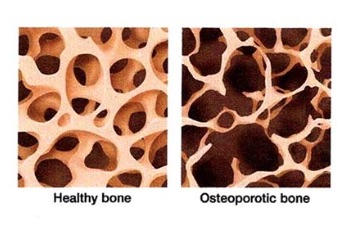
What’s The Difference Between Osteoporosis and Osteoarthritis?
Osteoporosis affects the bones. It is a decrease in bone density. The amount of bone is reduced and therefore the bones appear ‘holey’ on the inside. Osteoarthritis is a systemic disease, which means is affects all the bones in the body! It is not painful, but it can lead to a fracture!
Osteoarthritis affects the joint. The joints most commonly affected are the weight-bearing joints (hips, knees) and the joints we use often (like the fingers). Osteoarthritis is a degenerative condition that involves the thinning of the cartilage in the joints that can be painful, limit range of motion and affect activities of daily living.
Risk Factors for Developing Osteoporosis
Predicting who will, and who will not, develop osteoporosis has proven to be tricky. It is not uncommon for some individuals with no known risk factors to develop the disease. Some of the known risk factors are:
- female
- age (over 65)
- low body weight
- past fragility fracture
- having a family member with osteoporosis
- prolonged use of certain medications (example- prednisone, breast and prostate cancer drugs, depo-provera and others)
How To Get Tested For Osteoporosis
A bone mineral density test (BMD) is how healthcare providers can test for osteoporosis, or osteopenia, which is the early stage of the disease. A DEXA scan will be completed to test the bones and see how strong they are. The scan is painless and does not require any injections. It is basically an x-ray (so there is a low dose of radiation associated with the test) that scans the spine and hips to test how dense the bones are.
Your family doctor will refer you for this testing.
Who Should Get Tested?
- All women and men 65 years or older
- Postmenopausal women and men 50 – 64 with risk factors for fracture including:
- Fragility fracture after age 40
- Vertebral fracture or low bone mass identified on x-ray
- Parental hip fracture
- High alcohol intake
- Current smoking
- Low body weight (less than 132 lbs or 60 kg)
- Weight loss since age 25 greater than 10%
- High risk medication use: prolonged glucocorticoid use, aromatase inhibitors for breast cancer, androgen deprivation therapy for prostate cancer
- Rheumatoid arthritis
- Other disorders that may contribute to bone loss
- Younger men or women (under 50) with a disease or condition associated with low bone mass or bone loss:
- Fragility fractures
- High-risk medication use (steroid use, aromatase inhibitors, androgen deprivation therapy)
- Rheumatoid arthritis
- Other chronic inflammatory conditions
- Cushing’s disease
- Malabsorption syndrome
- Uncontrolled hyperthyroidism
- Primary hyperparathyroidism
- Hypogonadism; Early menopause (< 45 years old)
- Other disorders associated with rapid bone loss/fractures
So now that we know a little bit more about osteoporosis, let’s learn what we can do to help.
Managing Osteoporosis
Diet
A nutrient-rich diet is an important tool when managing osteoporosis. When it comes to bone health, there are two really important nutrients; calcium and vitamin D.
Calcium
Calcium is always the major nutritional component that goes hand-in-hand with discussing osteoporosis. In individuals with osteoporosis, proper calcium intake can slow bone loss and help prevent fractures.
As we get older, we don’t absorb calcium from our foods as effectively as we did when we were younger, so making sure that there is Milk and dairy products are the simplest ways to meet the daily recommended intakes. Have a dairy allergy? No problem! Broccoli, edamame, bok choy, almonds, figs and oranges are all good sources of calcium too! Calcium supplements are also available if you find it difficult to get the required intake through food sources alone!

Vitamin D
The other especially important vitamin when dealing with osteoporosis is vitamin D. Vitamin D helps our bodies absorb calcium from the food we ingest. Here in Canada, we don’t get as much sun as our bodies would like, and the sun is our best source of vitamin D. There are some food sources of vitamin D available; the most rich sources are swordfish, salmon, snapper, milk and soy beverages. For this reason, many people turn to supplements to meet the daily recommended intake of this very important vitamin.
Osteoporosis Supplements
Supplements are often a quick and easy way to get the recommended dose of vitamins and minerals. Experts always suggest obtaining these vitamins through food sources, but if that’s not an option, supplements can help!
For calcium, the daily recommended intake is 1000mg for people 19-50 years old, women who are pregnant and and women who are breastfeeding. People older than 50 require a higher daily intake of 1200mg.
For vitamin D, the daily recommended intake for people 19-50 years old require 400-1000 IU daily. Pregnant and women who are breastfeeding also require 400-1000 IU daily. For individuals over 50 years old the recommended intake increases to 800-2000 IU daily.
Exercise
Exercise is so important in managing osteoporosis. There are a few different aspects that are especially important.
Weight-bearing Exercise
Weight-bearing exercises are key! The impact from weight-bearing can actually stimulate your body to build new bone and therefore make your bones stronger! When we increase the demand on our bones (through impact exercise) our bodies respond by laying down more bone. This helps counteract the bone loss that occurs in osteoporosis! Some examples of great weight-bearing exercises are walking, hiking, dancing, tennis, aerobics and jogging.
Muscle Strengthening Exercises
Keeping the muscles strong is important, especially in our later years. Using resistance bands or weights is a safe and effective way to strengthen muscles and help keep the body fit. Strengthening should be incorporated 2-3 times a week. Keeping the muscles strong helps reduce the chance of falls which is important when the bones are more fragile!
Learn More About Strength Training Here
Balance Exercises
Balance is the last piece of the exercise puzzle. Actively working to improve balance will help avoid falls – which can have devastating consequences for people with osteoporosis. Some simple balancing exercises should be completed every day to minimize the risks of a falls. Yoga and tai chi are also excellent options for improving balance. A few minutes of daily balance exercises can be the difference between a healthy life and a broken hip!
Preventing Osteoporosis
Being proactive and following the management guidelines before being diagnosed with osteoporosis is, by far, the best idea. Getting regular exercise and focusing on a diet of nutrient rich foods is beneficial for preventing osteoporosis before it becomes a problem. Following the management guidelines can also help slow down the osteoporosis process, and keep the disease from progressing.
If you’re looking for some recipes to help plan meals that are good sources of vitamin C and calcium, the National Osteoporosis Foundation has some great bone-health recipes to try! The International Osteoporosis Foundation also offers some great recipes that promote good bone health and help prevent and manage osteoporosis.
Fall Prevention
For seniors over the age of 70, osteoporosis becomes an inevitability, and proper management is of the utmost importance. Balance and stability become major issues as the years advance, and slips/falling with osteoporosis can be life altering. The risk of fracture is much higher in individuals with osteoporosis, and breaking a hip/pelvis can be extremely dangerous.
Learn More About How Chiropractic Can Help Prevent Falls
There are also programs designed for seniors to specifically address fall prevention. The Oakville Trafalgar Memorial Hospital offers a falls prevention program. Individuals over the age of 65, living within the Oakville community and experiencing falls are eligible to take part in the Fall Prevention Clinic. There are other programs in Oakville that offer fall prevention workshops and courses. Click here for a list of other community resources.
Fall Prevention Tips
There are some simple tips to help avoid falls both inside and outside of the home.
- Wear low heeled shoes with rubber soles for better grip on potentially slippery surfaces
- Always use hand rails on the stairs
- Install grab bars in the bathroom to avoid slips on tile floors
- Limit using rugs around the home, tripping over the corners/edges is a major cause of falls
- If your doctor or chiropractor has recommended that you use a walker or cane, USE IT
- Always keep your driveway, porch and sidewalks cleared of leaves and snow
- Keep areas well lit, it’s easy to trip over things you can’t see
- Keep floors and high-traffic areas free of clutter
- If you live alone, carry your phone or Personal Emergency Response System with you at all times, so that you can call for help in case of an emergency
- Be careful when travelling up and down curbs. Take your time, examine the height and proceed with caution. Even small curbs can be extremely problematic!