Piriformis Syndrome Treatment Oakville
If you are searching for piriformis syndrome treatment in Oakville because of deep buttock pain that shoots, burns, tingles, or travels down the back of the thigh, you are not alone. Piriformis syndrome is a common cause of buttock and leg pain that is frequently mistaken for other lower back conditions. At Nottinghill Family Wellness Centre in Oakville, our chiropractors and physiotherapy team regularly assess patients experiencing this pattern of pain and nerve irritation.
Piriformis syndrome occurs when the piriformis muscle, located deep in the gluteal region, irritates or compresses the nearby sciatic nerve. This can produce symptoms that feel similar to sciatica, including buttock pain, tingling in the leg, or discomfort when sitting, walking, or climbing stairs. However, unlike lumbar disc injuries, the irritation in piriformis syndrome often originates in the deep hip muscles rather than the lower spine.
Piriformis syndrome occurs when the piriformis muscle in the deep gluteal region irritates the sciatic nerve, causing pain that often travels from the buttock down the leg.
Many patients seeking piriformis syndrome treatment in Oakville, Burlington, Milton, and Mississauga are surprised to learn that their symptoms may be coming from tight or overloaded gluteal muscles rather than a spinal problem.
This page explains what piriformis syndrome is, why it develops, what symptoms it commonly causes, and how our clinic approaches treatment using conservative, evidence based therapies designed to restore normal muscle function and reduce irritation of the sciatic nerve.
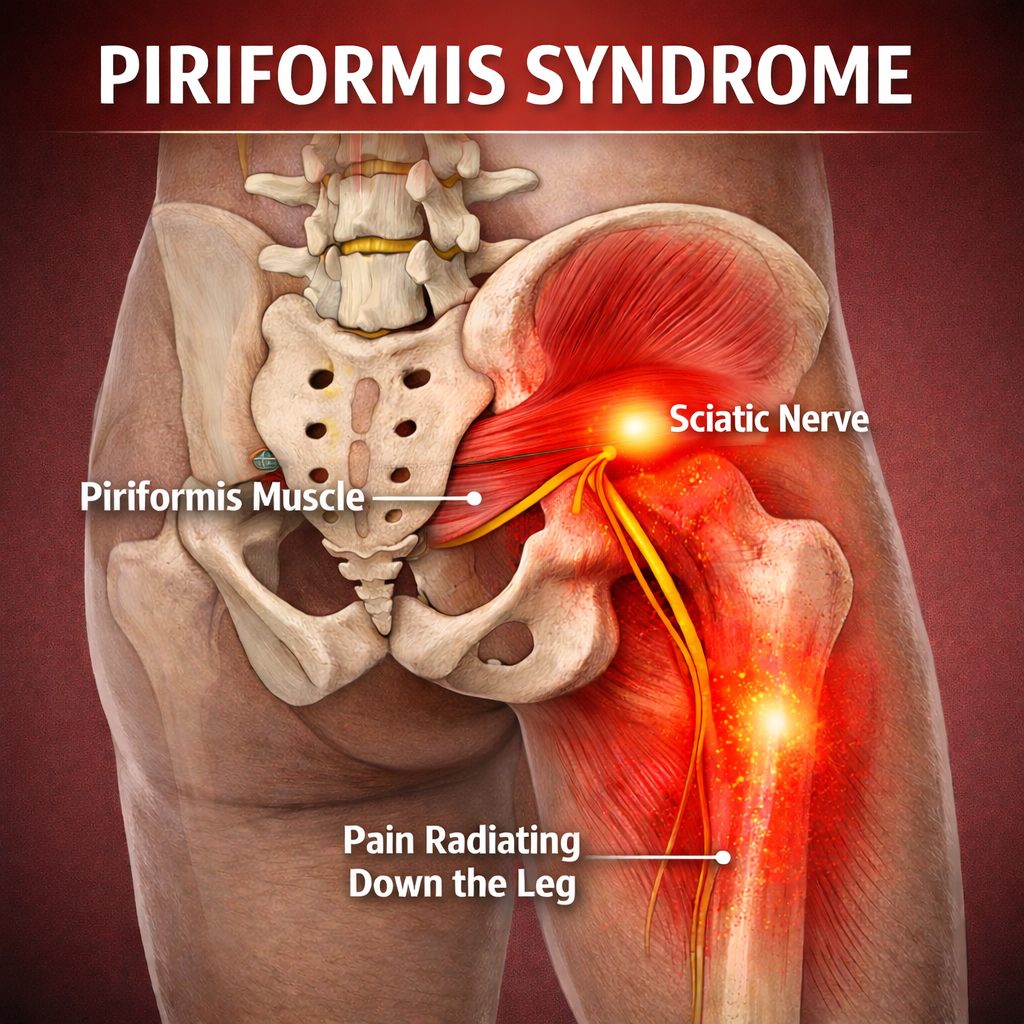
Piriformis Syndrome vs Herniated Disc
Many patients searching for piriformis syndrome treatment in Oakville are experiencing symptoms that can also occur with other conditions affecting the lower back and sciatic nerve. Pain that travels from the buttock into the back of the thigh, tingling in the leg, or discomfort when sitting for long periods can sometimes look very similar whether the irritation is coming from the piriformis muscle or from a lumbar disc in the spine.
Because these symptoms overlap, a careful clinical examination is important to determine the true source of the problem. At our clinic, this includes reviewing the patient’s history, assessing movement of the lower back and hips, performing orthopedic and neurological testing, and evaluating the surrounding muscles of the gluteal region.
This process helps identify whether the sciatic nerve irritation is being caused by the piriformis muscle itself, a lumbar disc herniation, or another structure in the lower back, allowing treatment to be directed at the actual source of the pain.
Many patients from Burlington visit our Oakville clinic for assessment and treatment of piriformis syndrome and deep gluteal muscle pain. Because piriformis irritation can mimic other causes of leg pain, a careful examination helps determine whether the symptoms are coming from the piriformis muscle or another structure affecting the sciatic nerve.
What Causes Piriformis Syndrome?
Piriformis syndrome usually develops when the piriformis muscle becomes tight, reactive, and mechanically “sticky” — and starts irritating the nerve (or nearby nerve structures) as it runs through the deep glute region.
Common contributors we see in Oakville patients with piriformis syndrome:
- Prolonged sitting (desk work, driving, long commutes)
- A sudden increase in walking, running, or hills/stairs
- Heavy lifting with twisting (especially when tired)
- Glute weakness and poor hip control (the piriformis “overworks”)
- Old low back/SI joint issues that change hip mechanics
- Hip stiffness (especially loss of internal rotation)
- Over training, sprinting, or return-to-sport too fast
- A fall or direct trauma to the glute/hip
- Wallet sitting (yes… it still matters for some people)
- Pregnancy/postpartum pelvic changes (common trigger)
- Leg length / gait issues that repeatedly overload one side
- Bad shoes are a major contributor
At our clinic, we don’t guess. We examine movement, irritability, hip rotation, nerve tension, and loading tolerance — then build a personalized treatment plan based on what your body is actually doing to cure your piriformis syndrome.
Piriformis Syndrome Treatment in Oakville: What You Need to Know
A lot of people try to stretch the piriformis muscle, foam roll it, or “massage it harder”… and it flares up worse.
Why? Because piriformis syndrome is often a combination of:
- Irritated tissue (inflammation / sensitivity)
- Restricted glide (scar tissue / adhesions)
- Poor blood flow in stubborn chronic cases
- Weak or under-recruited glute med/max
- A cranky low back / pelvis that keeps re-triggering it
So, the most effective plan is comprehensive: calm it down, restore tissue motion, improve circulation, correct joint mechanics, and rebuild control — in that order.
That’s exactly why our in-clinic protocol stacks therapies the way it does.
Who gets piriformis syndrome?
Piriformis syndrome commonly affects runners, cyclists, individuals who sit for long periods, and patients recovering from lower back injuries.
What Is Piriformis Syndrome? Piriformis Pain Relief!
The piriformis is a small but powerful muscle deep in your buttock. It runs from the sacrum (tailbone area) to the top of the femur (thigh bone) and helps with hip rotation and stability.
When it gets overloaded, it can:
- Feel like a deep ache or knot in the glute
- Refer pain down the back of the leg
- Feel worse with sitting, driving, or getting up from a chair
- Feel worse with stairs, hills, or longer walks
- Sometimes create tingling/numbness (not always)
Common Piriformis Syndrome Symptoms
- Deep buttock pain (often one side)
- Pain that spreads into hamstring / calf (sometimes)
-
Tightness in hip, glute, hamstring
-
Pain when sitting longer than 10–30 minutes
-
Pain rolling over in bed or sleeping on that side
-
A sharp “grab” when standing up after sitting
-
Pain with squats, lunges, or bending (sometimes)
Important note (and why the exam matters)
Not every “piriformis” case is piriformis syndrome. Some are:
-
Hamstring tendon problems
- Lumbar Stenosis
That’s why we treat this like healthcare should be done: skilled, qualified professional healthcare experts, using an evidence-based assessment — not just chasing symptoms.
6 Steps to Effective Piriformis Syndrome Treatment in Oakville
Our piriformis protocol focuses on reducing pain, restoring hip + pelvis mechanics, and getting the sciatic nerve to calm down. Treatment commonly includes Suction IFC + Heat, Shockwave Therapy, ART, chiropractic adjustments, instrument-assisted soft tissue therapy, and a very specific at-home exercise progression.
Step 1. Suction Interferential Current Therapy (IFC) + Moist Heat
Most piriformis cases start with pain sensitivity and guarding. We begin by calming the nervous system and improving circulation.
Why we do IFC and HEAT first:
-
Decreases pain signals and protective spasm
-
Improves blood flow to deep glute tissue
-
Makes shockwave and hands-on work dramatically more tolerable
-
Helps the muscle stop “clenching” around the area
Moist heat layered with IFC helps “open the door” so the rest of treatment actually works. This is part of why patients often feel looser right after the first visit. IFC is an electrical stimulation machine that promotes blood flow and healing.
Patients from Milton frequently seek treatment for persistent buttock pain, hip tightness, and leg symptoms related to piriformis syndrome. Our clinic provides conservative treatment approaches designed to reduce muscle tension, restore normal hip movement, and decrease irritation of the nearby sciatic nerve.

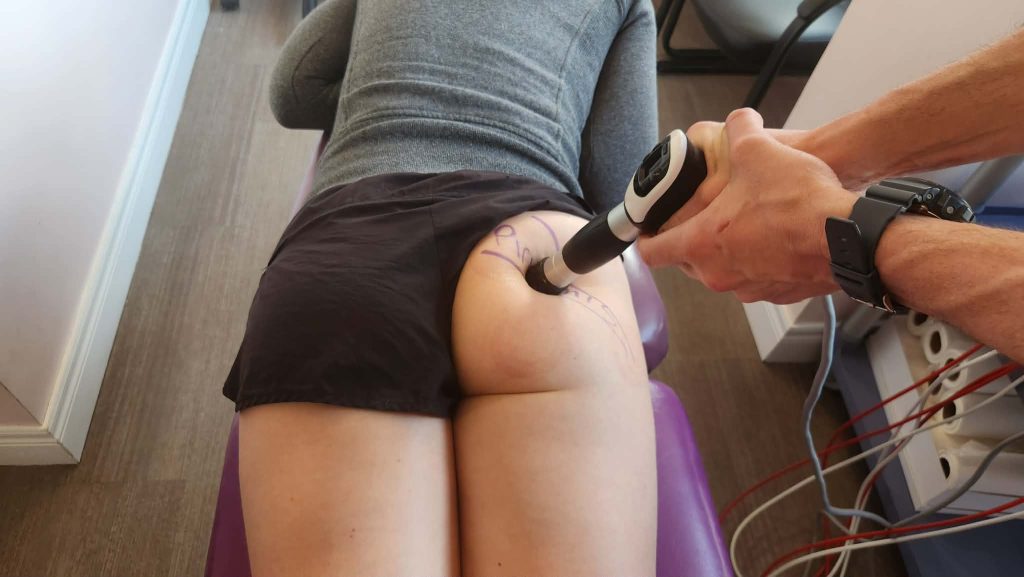
Step 2. Shockwave Therapy for Piriformis Syndrome Oakville
Shockwave is one of the most useful tools we have for stubborn deep glute and posterior hip pain — especially when the tissue has been irritated for weeks/months and doesn’t respond to stretching alone. Shockwave is an air powered gun that shots a bullet 15 x a second for up to 1800 hits. Dr. Steve and his staff use a special applicator head to get the shockwave machines mechanical and sound energy to penetrate up to 55mm, to get the deep deep tissues of your bum and hip.
What shockwave helps with:
-
Breaking up chronic adhesions/scar tissue patterns
-
Stimulating healing and circulation (new micro-blood flow response)
-
Desensitizing the area so it stops flaring with basic movement
-
Improving glide between muscle layers (huge for deep glute pain)
This is state-of-the-art care when used properly — not “randomly blasting the butt.” We treat specific lines of tension based on your exam and symptoms.
Step 3. Instrument-Assisted Soft Tissue Therapy (IASTT) — Hamstrings + Lower Glute
After shockwave, we often use instrument-assisted work (yes, the “scraping” tool) — but for piriformis syndrome we typically focus more on the lower glute, hamstring origin, and the tissue pathways that refer down the leg.
Why this matters:
Piriformis syndrome rarely lives in one tiny spot. Tight hamstrings and lower glute adhesions can keep pulling the hip into patterns that re-trigger the piriformis.
IASTT:
-
helps release “stuck” tissue planes
-
improves range of motion
-
reduces that constant “pull” sensation
-
can make sitting and walking feel easier quickly
You’ll usually get icing instructions afterwards if you’re sore — because the goal is a controlled stimulus that helps the body remodel, not a bruised mess.
Step 4. Active Release Therapy (ART) — Deep Glute + Hip Rotators
ART is hands-on, movement-based soft tissue treatment. For piriformis syndrome, it’s one of the best ways to restore normal length and motion in the deep hip rotators while your hip moves through positions that usually trigger symptoms.
What we’re targeting:
-
piriformis
-
deep glute rotators
-
glute max/med tension patterns
-
hip capsule restrictions that force compensation
This is where the “knot” starts to let go — and where patients often notice their leg symptoms calm down.
Step 5. Chiropractic Adjustment (Low Back / Pelvis / SI Joint / Hip — as needed)
Here’s the truth: many piriformis syndromes are sustained by joint mechanics. If the pelvis, SI joint, or low back is moving poorly, the piriformis will often tighten to stabilize the area. Chiropractic adjustments can help!
We adjust only what needs it, after the tissue is prepared (that’s why steps 1–4 come first).
Why this helps:
-
restores joint motion that the piriformis was compensating for
-
decreases protective tone in the deep glute
-
improves hip rotation and stride mechanics
-
reduces recurrence
This is where our approach is optimized: treat the tissue + correct the joint driver + reinforce with rehab.
Patients from Mississauga often visit our Oakville clinic when piriformis syndrome symptoms interfere with sitting, walking, or physical activity. Identifying tight or dysfunctional gluteal muscles can help guide treatment that focuses on restoring normal muscle function and reducing nerve irritation.
Meet Our Team
Step 6. At-Home Exercises (This is the difference-maker)
If piriformis syndrome has been hanging around, exercises aren’t optional — they’re the part that keeps you from coming back every time you sit too long or do a big walk. Exercises to prevent piriformis syndrome are the corner stone of our treatment program!
We keep it simple and progressive. The goals are:
-
restore hip internal rotation control
-
strengthen glute med/max so piriformis stops overworking
-
improve pelvic stability during walking/stairs
-
calm the nerve sensitivity with graded loading
Typical “starter” home plan (we tailor to you):
-
Gentle glute activation (bridges, isometrics, side-lying holds)
-
Hip mobility work (targeted, not aggressive stretching)
-
Nerve-friendly movement (walking dosage, positional breaks from sitting)
-
Progression to step-ups, split squats, banded hip control
-
Return-to-run or sport progression when appropriate
You’ll get a plan that matches your irritability level — backed by science and evidence, not random YouTube rehab.
What Our Patients Are saying
How to Prevent Piriformis Syndrome Flare-Ups
Piriformis syndrome often comes back when the same stress pattern returns. Prevention is usually about fixing the daily triggers:
Sitting strategy
-
Break up sitting every 20–40 minutes
-
Avoid deep slouched sitting (posterior pelvic tilt)
-
Use a small lumbar support in the car if driving is a trigger
Build glute endurance
-
Glute med endurance is the “anti-piriformis overload”
-
Consistency beats intensity (2–4 short sessions/week)
Warm up before hills / runs / heavy days
-
A 3–5 minute activation warmup can prevent flare-ups
Don’t stretch it aggressively when it’s angry
-
Early on, too much stretching can poke the bear
Can Our Oakville Physiotherapy Team Treat Piriformis Syndrome?
Yes. If you’re nearing the end of chiropractic coverage (or you prefer physiotherapy), our Oakville physiotherapy team can treat piriformis syndrome using the same core principles: evidence-based assessment, hands-on therapy, and exercise progression.
At Nottinghill Family Wellness Centre, our providers work as a team — so your plan stays consistent and coordinated, with a personalised treatment plan that fits your goals.
Piriformis Syndrome FAQS
What is piriformis syndrome and how does it cause sciatica?
Piriformis syndrome occurs when the piriformis muscle deep in the buttock becomes tight or irritated and compresses the nearby sciatic nerve. This can cause pain in the buttock that may radiate down the back of the leg, often mimicking sciatica from the low back. At our Oakville clinic, our chiropractor performs a detailed assessment to determine whether your symptoms are coming from the piriformis muscle, the lumbar spine, or another structure before creating a personalised treatment plan.
What are the most common symptoms of piriformis syndrome?
Piriformis syndrome typically causes deep buttock pain that may spread down the back of the thigh. Many Oakville patients describe burning, tingling, or numbness along the sciatic nerve pathway. Symptoms are often worse when sitting for long periods, driving, climbing stairs, or getting up from a seated position.
What causes piriformis syndrome?
Piriformis syndrome can develop from prolonged sitting, repetitive hip movements, sports injuries, lifting with twisting motions, or poor hip and glute strength. Many Oakville patients develop piriformis irritation from long commutes, desk work, running, or sudden increases in physical activity.
How is piriformis syndrome diagnosed?
Diagnosis begins with a physical examination of the lower back, pelvis, and hip to determine the true source of sciatic nerve irritation. Our Oakville chiropractor evaluates hip rotation, nerve tension, muscle tightness, and joint movement to determine if the piriformis muscle is compressing the sciatic nerve or if symptoms are coming from the lumbar spine or sacroiliac joint.
Can chiropractic treatment help piriformis syndrome?
Yes. Chiropractic treatment can be very effective for piriformis syndrome when the underlying cause involves joint dysfunction in the pelvis, sacroiliac joint, or lower back. At our Oakville clinic, chiropractic adjustments are often combined with shockwave therapy, Active Release Therapy, and soft tissue treatment to reduce muscle tension and restore proper movement.
Does shockwave therapy help piriformis syndrome?
Shockwave therapy is commonly used at our Oakville clinic to treat chronic piriformis syndrome. Shockwave therapy helps stimulate blood flow, reduce chronic inflammation, and break up scar tissue in the deep glute muscles. This can significantly reduce pressure on the sciatic nerve and accelerate recovery.
How long does piriformis syndrome take to heal?
Recovery time depends on how long symptoms have been present and what factors caused the irritation. Many Oakville patients begin to notice improvement within a few treatments when the piriformis muscle is properly addressed with a comprehensive treatment plan that includes hands-on therapy and corrective exercises.
What exercises help piriformis syndrome?
Exercises for piriformis syndrome typically focus on improving hip mobility, strengthening the glute muscles, and reducing strain on the piriformis muscle. Our Oakville clinic provides patients with personalized home exercise programs designed to improve stability and prevent future flare-ups.
When should I seek treatment for piriformis syndrome?
If buttock pain or sciatic-type symptoms persist for more than a few days, worsen with sitting, or begin to travel down the leg, it is a good idea to seek assessment. Early treatment at our Oakville clinic can help reduce irritation of the sciatic nerve and prevent the condition from becoming chronic.